A gynaecological cancer diagnosis can be a profound and challenging experience, often bringing with it a whirlwind of emotions and uncertainties. These cancers, which affect the female reproductive organs, including the cervix, ovaries, uterus, vagina, and vulva, impact countless lives globally. Facing such a diagnosis requires courage and, crucially, accurate information to navigate the path forward.
This guide provides a clear and comprehensive overview of treatment for gynaecological cancer, outlining the various options available to help patients make informed decisions about their care. The goal is to empower individuals with knowledge, helping them understand the approaches their healthcare team may discuss and why certain treatments are chosen. At the same time, it serves as a reminder that continued advancements in medical science are not only expanding treatment possibilities but also offering renewed hope, hope for better outcomes, improved quality of life, and a more confident path forward.
Understanding Gynaecological Cancers
What are Gynaecological Cancers?
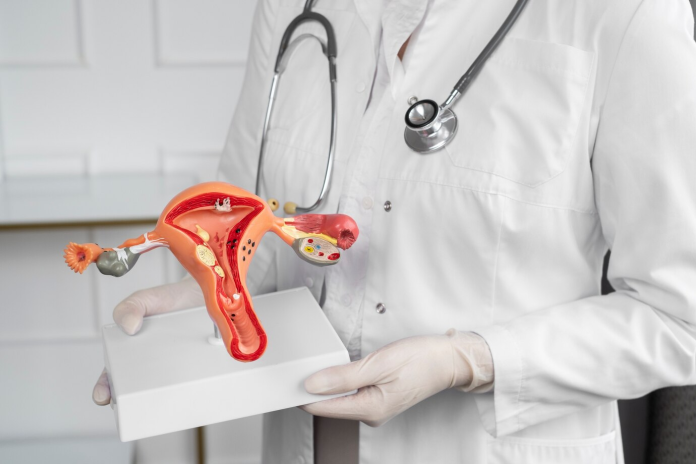
Gynaecological cancers are a group of diverse malignancies that originate in the female reproductive system. Each type presents its own unique characteristics, requiring specific diagnostic and treatment approaches. The primary types include:
- Cervical Cancer: This cancer develops in the cervix, the lower, narrow part of the uterus that connects to the vagina. It is often linked to persistent infection with certain types of human papillomavirus (HPV).
- Ovarian Cancer: Originating in the ovaries, the two small glands on either side of the uterus that produce eggs and hormones. Ovarian cancer is often diagnosed at a later stage due to its subtle symptoms.
- Uterine (Endometrial) Cancer: This is the most common type of gynaecologic cancer, forming in the lining of the uterus, known as the endometrium. It often presents with abnormal vaginal bleeding.
- Vaginal Cancer: A rare cancer that begins in the vagina, the muscular tube connecting the uterus to the outside of the body.
- Vulvar Cancer: This cancer forms on the outer part of the female genitals (the vulva), typically presenting as a lump or sore.
Importance of Early Detection
Early detection plays a pivotal role in the successful treatment of gynaecological cancers. Many of these cancers, when identified in their early stages, are more amenable to effective intervention, leading to significantly better outcomes. For instance, regular cervical screening (often referred to as a “Peripheral Smear Test“) can detect precancerous changes or early-stage cervical cancer, allowing for timely treatment. Similarly, being aware of and reporting persistent symptoms such as abnormal bleeding, pelvic pain, or changes in bowel or bladder habits can prompt earlier investigation for other gynaecological cancers.
Factors Influencing Treatment Decisions
The development of a personalised treatment plan for gynaecologic cancer is a meticulous process, taking into account a range of crucial factors, including:
- Type of Cancer: Each specific gynaecologic cancer responds differently to various treatments.
- Stage of Cancer: This refers to the extent of the cancer’s spread – whether it’s confined to its original location, has spread to nearby tissues, or has metastasised to distant parts of the body. Staging is a critical determinant of treatment intensity and approach.
- Overall Health and Medical History of the Patient: Pre-existing health conditions, age, and general fitness all influence the suitability and tolerability of certain therapies.
- Patient Preferences and Goals: The patient’s wishes, especially regarding aspects like fertility preservation or quality of life, are paramount and will be integrated into the treatment discussion.
Cornerstone Treatment Modalities
Treating gynaecologic cancer often involves a combination of therapies, carefully chosen and sequenced to offer the best possible outcome for each patient. These approaches are continually refined through ongoing research and clinical advancements.
Surgery
Surgery is frequently the primary treatment for many gynaecological cancers, with the aim of removing as much of the cancerous tissue as possible. The specific surgical procedure will depend on the type, stage, and location of the cancer, as well as the patient’s overall health and desire for fertility preservation.
Minimally Invasive Surgery: Modern surgical techniques often allow for less invasive procedures.
- Laparoscopic Surgery: Involves making several small incisions through which a thin, lighted tube with a camera (laparoscope) and surgical instruments are inserted.
- Robotic-Assisted Surgery: Utilises a robotic system controlled by the surgeon to perform the operation with enhanced precision and dexterity through small incisions.
Benefits: These approaches often lead to smaller scars, reduced pain, shorter hospital stays, and quicker recovery times compared to traditional open surgery.
Open Surgery: This involves a single, larger incision to access the affected area. It is typically employed for more extensive cancers or when minimally invasive techniques are not suitable.
Specific Surgical Procedures:
- Hysterectomy: The removal of the uterus, and often the cervix. This can be partial (removing part of the uterus) or total.
- Oophorectomy: The surgical removal of one or both ovaries.
- Salpingectomy: The removal of one or both fallopian tubes.
- Lymph Node Dissection: Removal of lymph nodes (small glands that are part of the immune system) in the pelvis or abdomen to check if cancer has spread. This helps determine the cancer’s stage and guides further treatment.
- Debulking Surgery: Often performed for advanced ovarian cancer, this procedure aims to remove as much of the visible tumour as possible, even if it cannot remove all of it. This can make subsequent treatments like chemotherapy more effective.
- Vulvectomy: The removal of part or all of the vulva, typically for vulvar cancer. This can range from a wide local excision (removing only the cancerous area and a margin of healthy tissue) to a radical vulvectomy (removing larger sections of the vulva).
- Vaginectomy: The surgical removal of part or all of the vagina, performed for vaginal cancer.
- Fertility-Sparing Options: For some patients, particularly those with early-stage gynaecologic cancers who wish to preserve their ability to have children, specific surgical techniques may be considered. Examples include a radical trachelectomy for early cervical cancer, which removes the cervix but leaves the uterus intact, or unilateral oophorectomy for certain early-stage ovarian cancers affecting only one ovary.
Radiation Therapy
Radiation therapy, also known as radiotherapy, uses high-energy rays or particles to destroy cancer cells and shrink tumours. It can be used as a primary treatment, following surgery (adjuvant therapy), before surgery (neoadjuvant therapy) to shrink tumours, or to manage symptoms.
- External Beam Radiation Therapy (EBRT): This is the most common type, where a machine outside the body directs a beam of radiation to the area affected by cancer. Treatment is typically delivered in short, daily sessions over several weeks.
- Brachytherapy (Internal Radiation): Involves placing a radioactive source directly inside or very close to the tumour. This allows for a very high dose of radiation to be delivered to the cancer while sparing surrounding healthy tissues. Brachytherapy can be temporary (source removed after a short period) or permanent (source remains in the body).
Chemotherapy
Chemotherapy uses powerful medications to kill cancer cells or stop them from growing. These drugs typically travel throughout the bloodstream, targeting rapidly dividing cells, which include cancer cells. It can be given intravenously (through a vein), orally (as a tablet), or sometimes directly into a specific body cavity.
How it Works: Chemotherapy works by interfering with the growth and division of cancer cells. While effective, it can also affect healthy, fast-growing cells (like those in hair follicles, bone marrow, and the digestive system), leading to side effects.
When Is it Used: Chemotherapy may be administered:
- After surgery (adjuvant chemotherapy): To eliminate any remaining cancer cells and reduce the risk of recurrence.
- Before surgery (neoadjuvant chemotherapy): To shrink a tumour, making it easier to remove surgically.
- As a primary treatment: For cancers that are more widespread or cannot be removed surgically.
- For recurrent or advanced disease: To control symptoms and prolong life.
Intraperitoneal Chemotherapy: For certain gynaecologic cancers, particularly advanced ovarian cancer, chemotherapy drugs can be delivered directly into the abdominal cavity (peritoneum). This allows for a higher concentration of the drugs to reach cancer cells within the abdomen.
Targeted Therapy
Targeted therapies are a newer class of drugs that work by specifically attacking certain molecules or pathways within cancer cells that are essential for their growth, division, and spread. Unlike traditional chemotherapy, they are designed to be more precise, often leading to fewer side effects on healthy cells.
Mechanism: These treatments identify and block specific ‘targets’ in cancer cells. For example:
- Some drugs can block the signals that tell cancer cells to grow and divide uncontrollably.
- Others can inhibit the formation of new blood vessels (angiogenesis inhibitors) that tumours need to obtain nutrients and grow.
- PARP inhibitors (Poly ADP-ribose Polymerase inhibitors) are an example of targeted therapy used for certain gynaecologic cancers, particularly ovarian cancer with specific genetic mutations. They work by blocking a protein involved in repairing damaged DNA in cancer cells, leading to their death.
Immunotherapy
Immunotherapy is an innovative treatment approach that harnesses the power of the body’s own immune system to recognise and fight cancer. Instead of directly attacking cancer cells, these drugs stimulate the immune system to do the job.
- Mechanism: Cancer cells can sometimes evade the immune system by sending out signals that ‘switch off’ immune cells. Immunotherapy drugs, particularly checkpoint inhibitors, work by blocking these ‘off’ signals, effectively ‘releasing the brakes’ on the immune system, allowing it to recognise and attack the cancer cells.
- When Used: While still relatively new for many gynaecological cancers, immunotherapy is showing promise in certain types, especially for advanced or recurrent disease where other treatments may have been less effective.
Supportive Care and Side Effect Management
Undergoing treatment for gynaecological cancer can be physically and emotionally challenging. Alongside eradicating the cancer, managing treatment side effects and supporting overall well-being are vital components of comprehensive care. This holistic approach, often called supportive or palliative care, aims to improve quality of life throughout the cancer journey.
Managing Treatment Side Effects
Each treatment carries potential side effects, experienced differently by individuals. Healthcare teams work closely with patients to anticipate, prevent, and manage these effects.
Common side effects across modalities include fatigue, nausea and vomiting, and pain. Surgery might lead to pain at the incision site, limited mobility, or lymphoedema. Radiation therapy can cause skin irritation, bowel/bladder changes, or vaginal dryness/stenosis if targeting the pelvic area. Chemotherapy side effects can include hair loss, anaemia, increased infection risk due to lowered white blood cells, nerve damage (neuropathy), and mouth sores. It is crucial to tell the medical team about any new or worsening side effects promptly, as many can be effectively managed.
Holistic Support
Beyond physical symptoms, comprehensive care addresses cancer’s broader impact on life.
This includes dedicated pain management, nutritional support from a dietitian, and vital psychological and emotional support from counsellors or support groups to help manage anxiety and stress. Discussions about sexual health and intimacy are also important, addressing changes and exploring ways to maintain intimacy. Physical therapy or rehabilitation can aid in regaining strength and flexibility. Lastly, palliative care focuses on providing relief from the symptoms and stress of illness at any stage, not just end-of-life, to improve quality of life for both patients and their families.
Embracing a Future of Hope in Gynaecological Cancer Care
Today, advances in gynaecological cancer care offer more reason than ever to feel hopeful. With a growing range of effective treatment options—including surgery, radiotherapy, chemotherapy, targeted therapies, and immunotherapy—care is becoming increasingly precise and personalised. Every treatment plan is thoughtfully tailored to the individual, supported by experienced medical teams and comprehensive supportive care. As ongoing research continues to expand what’s possible, the outlook for those affected is brighter than ever—bringing the promise of better outcomes, improved quality of life, and renewed confidence in the journey ahead.